Causes Suicide:
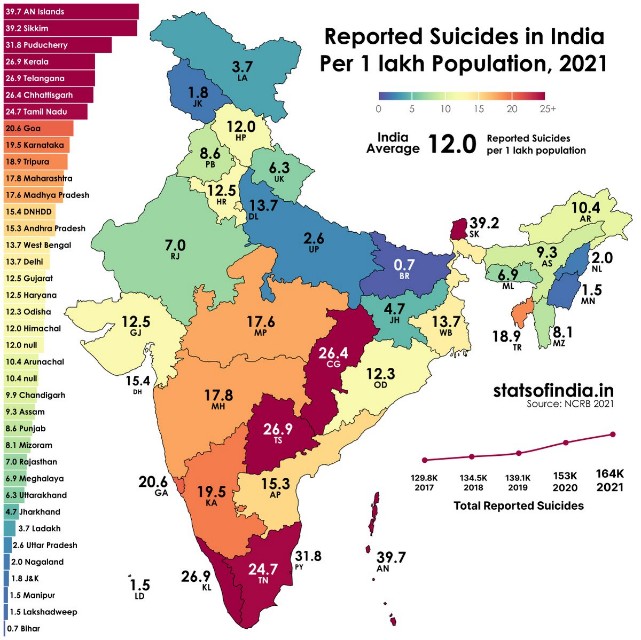
Spatial analysis of Suicide:
| Concept | Description / Explanation |
|---|---|
| DALY (Disability Adjusted Life Year) | Combined measure of years lost to illness, disability, or early death; quantifies overall disease burden. |
| Alzheimer’s Disease | Progressive, irreversible brain disorder causing memory loss, confusion, and cognitive decline. |
| Dementia | Group of conditions marked by decline in memory, reasoning, and thinking, impairing daily functioning. |
| Burnout Syndrome | Prolonged work-related stress leading to emotional exhaustion, detachment, and reduced professional efficacy. |
| Stepped Care | Treatment model where care intensity is matched to severity; escalates support only as needed. |
| District Mental Health Programme (DMHP) | Government initiative integrating mental health into district-level public healthcare, focusing on early detection, treatment, and community awareness. |
| Demographic / Region | Key Statistic or Fact |
|---|---|
| Prevalence | 13.7% overall; 15% among adults; 2% experience severe mental disorders. |
| Urban prevalence | 13.5% |
| Rural prevalence | 6.9% |
| High-risk age group | 18–30 years — accounts for approximately 35% of suicides. |
| Women | Experience higher stress levels and greater vulnerability to domestic violence. |
| Men | Represent 73% of suicide victims. |
| Treatment gap | 70–92% of individuals with mental illness remain untreated. |
| States with highest suicide rates | Andaman & Nicobar Islands, Sikkim, Kerala, Manipur. |
| States with large mental health burden | Maharashtra, Tamil Nadu, Madhya Pradesh, Karnataka, West Bengal. |
| Best service coverage | Kerala and Tamil Nadu. |
| Farmer suicide clusters | Maharashtra and Karnataka. |